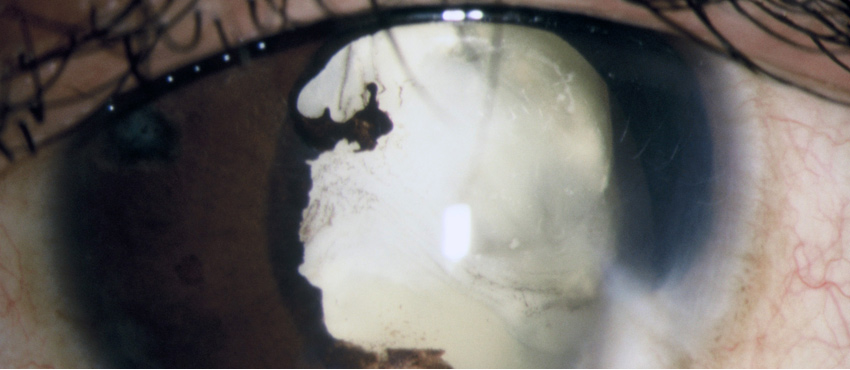
Causes
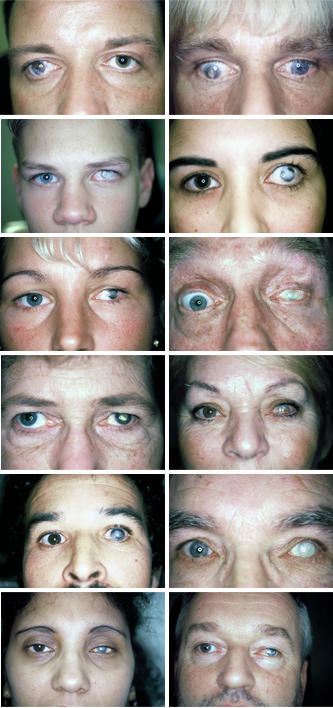
History
Some of the following methods for treating damaged corneas are still being used in ophthalmology. The results are often disappointing. (see below)
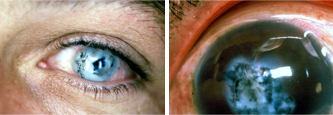
Cornea injected with black ink, followed by the application of platinumchloride to create the shape of a pupil.
Cornea injected with black ink.
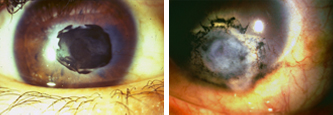
Ironsulphate and 5% tannic acid.
Treated with platinumchloride and 5% tannic acid.
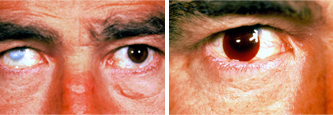
Untreated eye.
Coloured bandage lens on untreated eye.
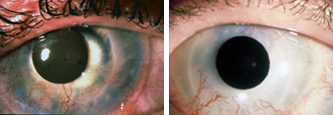
Bandage lens as pupil.
Bandage lens as pupil.




Links

Cornea damage
Introduction
When the cornea is damaged, the patient usually has to deal with 3 disturbing consequences. Whereas the cosmetic side is obvious, the psychological and physiological effects are very often underestimated.
Throughout the history, there has always been discrimination against people with damaged corneas. Most people experience discolouration of the cornea as disturbing and many cultures shun people with “the evil eye”. In western cultures patients also suffer and can be the victim of disturbing reactions, which makes them feel insecure. Sometimes it can be severe enough to cause psychological problems that complicate their social interactions.
Throughout the history, there has always been discrimination against people with damaged corneas. Most people experience discolouration of the cornea as disturbing and many cultures shun people with “the evil eye”. In western cultures patients also suffer and can be the victim of disturbing reactions, which makes them feel insecure. Sometimes it can be severe enough to cause psychological problems that complicate their social interactions.
Causes of corneal damage
There are various causes leading to corneal damage.
These can include:
● Splinters of wood, metal or glass.
● Sharp toys, pencils, paper arrows.
● Chemical burns (caused by acid or lye).
● Infections
● Too many cornea surgeries.
● Vitamin A deficiency. Due to poor nutrition which is common in underdeveloped/developing countries.
These can include:
● Splinters of wood, metal or glass.
● Sharp toys, pencils, paper arrows.
● Chemical burns (caused by acid or lye).
● Infections
● Too many cornea surgeries.
● Vitamin A deficiency. Due to poor nutrition which is common in underdeveloped/developing countries.
History
● One of the oldest known treatments for cornea damage is tattooing. Galenus already described a method for colouring white spots in the cornea black.
● Starting in the 1870’s, ophthalmologists have been trying to improve on the procedure of tattooing the cornea. Their aim was as follows:
● Colour light spots or scars (leucoma) on the cornea – especially disturbing when they are on the pupil or the dark coloured iris.
● Contouring of deformed pupils.
● Covering of cornea turbidities.
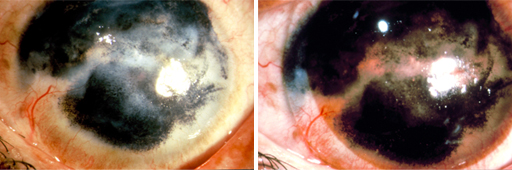
Intra-corneal injection with black ink, then place the the bandage lens. This method is still practiced.
● Mimicking the iris colour.
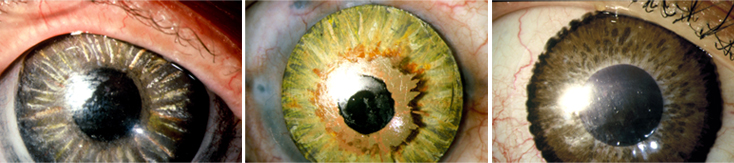
Using hand painted lenses.
● Replace the natural pigment in the cornea and conjunctiva (albinisme).
● Imitation of the cornea in shriveled eyes to replace a glass prosthesis.
● A lot of different instruments were used to add the pigments. To this day coloured corneas are treated worldwide by injecting Indian black ink, platinum chloride, hydrazinehydrate or ferro sulphate with 5% tannine acid.
● Until 1990 the results were bad: the pigments hardly stayed in place and were known to cause irritations and inflammations. Therefor a scale prosthesis was usually used in the second instance.
● Starting in the 1870’s, ophthalmologists have been trying to improve on the procedure of tattooing the cornea. Their aim was as follows:
● Colour light spots or scars (leucoma) on the cornea – especially disturbing when they are on the pupil or the dark coloured iris.
● Contouring of deformed pupils.
● Covering of cornea turbidities.

● Mimicking the iris colour.

● Replace the natural pigment in the cornea and conjunctiva (albinisme).
● Imitation of the cornea in shriveled eyes to replace a glass prosthesis.
● A lot of different instruments were used to add the pigments. To this day coloured corneas are treated worldwide by injecting Indian black ink, platinum chloride, hydrazinehydrate or ferro sulphate with 5% tannine acid.
● Until 1990 the results were bad: the pigments hardly stayed in place and were known to cause irritations and inflammations. Therefor a scale prosthesis was usually used in the second instance.
Treatment by an ophthalmologist
Nowadays an ophthalmologist will first try to preserve eye sight when treating the above mentioned cases of cornea damage. Unfortunately, this is not always successful. In 30% of all cases the patient is completely blind; in 70% there is some light perception, which is, as stated earlier on, mostly disturbing.
If surgery does not prove to be successful and provides no solution, the person can opt for his or her measurements taken for a scale prosthesis. This can be made in a specific colour, with or without a pupil.
Over the course of time, many patients have problems with the scale prosthesis and it has to be removed. Another disadvantage of the scale prosthesis is that it doesn’t stay in place. In some cases the patient can benefit from keratography treatment.
If surgery does not prove to be successful and provides no solution, the person can opt for his or her measurements taken for a scale prosthesis. This can be made in a specific colour, with or without a pupil.
Over the course of time, many patients have problems with the scale prosthesis and it has to be removed. Another disadvantage of the scale prosthesis is that it doesn’t stay in place. In some cases the patient can benefit from keratography treatment.
Research
As has been confirmed in research throughout the last 20 years, it is not commonly known that more than 73% of patients with a damaged cornea experience other physical complaints. Even though it is known as a blind eye, the damaged cornea often permits sharp light to (partially) filter in (photo phobia). This results in impaired vision by the healthy eye. Additionally, disturbed vision can cause headaches and fatigue.
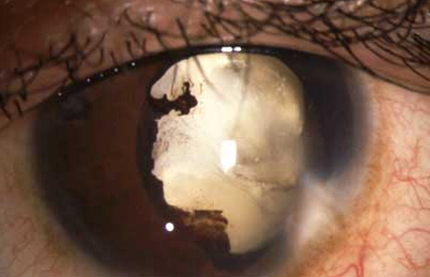
Patient with severe photofobia.
With the aid of keratography, these physical complaints often can be completely eradicated. Thanks to good cosmetic results, patients also experience a considerable overall psychological improvement, which improves their social interactions as well.

With the aid of keratography, these physical complaints often can be completely eradicated. Thanks to good cosmetic results, patients also experience a considerable overall psychological improvement, which improves their social interactions as well.
Keratography
Keratography is a scientifically founded method of permanently colouring the cornea with colour pigments. The founders of this sub-specialism, E.M. van der Velden and Dr. Jan Kok, laid the basis at AMC Oogheelkunde Amsterdam in 1990. It is known as keratography since 1995 (Prof. Dr. V. Claus, E.M. van der Velden).
In addition to outpatient treatment basis at the ophthalmology department of AMC, they focused on bacteriological, histopathological, electron-microscopic and röntgen-microanalysis research of the properties of the colour pigments to rule out any possible harmful side effects.
Through this research, they were able to prove that a number of the colour pigments are safe in treating the cornea.
Keratography was practiced by E.M. van der Velden at the Oogziekenhuis in Rotterdam (1995-2008), the Ludwig-Maximilian University (Ophthalmology) in Munchen (1996-2012), the Tilganga Eye Centre in Kathmandu in Nepal and the Clinic for Medical and Aesthetical Dermatography in Arnhem, The Netherlands.

In addition to outpatient treatment basis at the ophthalmology department of AMC, they focused on bacteriological, histopathological, electron-microscopic and röntgen-microanalysis research of the properties of the colour pigments to rule out any possible harmful side effects.
Through this research, they were able to prove that a number of the colour pigments are safe in treating the cornea.
Keratography was practiced by E.M. van der Velden at the Oogziekenhuis in Rotterdam (1995-2008), the Ludwig-Maximilian University (Ophthalmology) in Munchen (1996-2012), the Tilganga Eye Centre in Kathmandu in Nepal and the Clinic for Medical and Aesthetical Dermatography in Arnhem, The Netherlands.